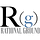Expert versus Expert
Michael Osterholm, a top health adviser to President Joe Biden, suggests the new strain of COVID may lead to future lockdowns. In a recent interview, Osterholm warned double-masking would be counterproductive and harmful—a stance that’s the complete opposite of the White House’s main adviser, Dr. Anthony Fauci.
Last Friday, Johnson & Johnson announced that its one-dose vaccine is 66% effective against moderate to severe COVID infection in a multicountry study. But importantly, it was 85% effective in protecting against severe disease. Johnson & Johnson expects to file with the FDA for an emergency use authorization this month.
In other news:
The Rational Grounds team is hosting a free webinar on Tuesday, February 9th at 9:30 pm ET/6:30 PT. We will share the tools and tactics you need to take back your school. Register here.
In a recent interview on the Megyn Kelly Show, Dr. Jay Bhattacharya, co-author of the Great Barrington Declaration, said the COVID lockdowns were an “overreaction” to “protect the rich.”
Nurse practitioner Christine Mathews says we must acknowledge the harmful psychosocial effects of the COVID lockdowns.
A new paper by Stanford epidemiologist John Ioannidis shows targeted protection of high-risk groups does work.
The pandemic has been hard on all kinds of relationships, but losing the incidental interactions with coworkers, neighbors, and friends of friends might be taking more of a toll than you realize, writes Amanda Mull in The Atlantic.
Israel's vaccination program is showing signs of working to drive down infections and illness in people over 60.
Interested in becoming knowledgeable on COVID? Become a premium member. Our premium members get special access to our personal data dashboards and analysis.
Want to support our work? Visit our Substack page and leave us a tip.
On Rational Ground for our premium members, our data analyses will always be available to you. Interested in becoming a COVID expert? Become a premium member.
Additionally, we just released an update on how COVID-19 is playing out on university campuses.
COVID News
Johnson & Johnson Covid-19 vaccine is 66% effective in global trial, but 85% effective against severe disease, company says
https://www.cnn.com/2021/01/29/health/johnson-coronavirus-vaccine-results/index.html
Johnson & Johnson's Covid-19 single-shot vaccine was shown to be 66% effective in preventing moderate and severe disease in a global Phase 3 trial, but 85% effective against severe disease, the company announced Friday.
The vaccine was 72% effective against moderate and severe disease in the US, the company said.
It's a striking difference from vaccines from Pfizer/BioNTech and Moderna, and it may give pause to people uncertain about which vaccine to get or when they can get one. The vaccines already on the market in the US are about 95% effective overall against symptomatic Covid-19, with perhaps even higher efficacy against severe cases.
But experts say the Johnson & Johnson vaccine will still be useful against the pandemic in the United States and around the world.
Biden Health Adviser Warns of Virus Variants, Future Lockdowns
A top health adviser to President Joe Biden warned Sunday that a new variant of the coronavirus circulating in the U.K. will likely become the dominant strain in the U.S. and may lead to future restrictions on in-person gatherings.
Michael Osterholm, director of the Center for Infectious Disease Research and Policy at the University of Minnesota, said on NBC’s “Meet the Press” that the nation’s health care system must prepare for a surge in serious cases such as the one experienced recently in England.
“What we have to do now is also anticipate this and understand that we’re going to have to change quickly,” said Osterholm, who’s a member of Biden’s Covid-19 advisory board. “As fast as we’re opening restaurants, we’re likely to be closing them in the near term.”
Osterholm: Double masking could lower your protection against COVID-19
A recommendation about double-masking by White House advisor Dr. Anthony Fauci isn't receiving any praise from one of the nation's leading experts on COVID-19.
Dr. Michael Osterholm, who leads the Center for Infectious Disease Research and Policy at the University of Minnesota, refuted Dr. Fauci's claim that double-layering would likely make masking "more effective."
"I do not support the idea of two masks," said Dr. Osterholm, who spoke to WCCO Radio's Cory Hepola on Wednesday morning.
Osterholm explained that masks work based on how they fit and their filtration.
"Masks, as they're defined work in two ways. The first is in regards to how that masks fits. How well does it fit around you? It's like swimming goggles. They don't usually leak through the lenses they leak through the seal around your eyes or face," said Osterholm.
Commentary/Analysis
COVID Vaccines, Masks and Schools, with Alex Berenson and Dr. Jay Bhattacharya
Megyn Kelly is joined by Alex Berenson, author and former New York Times reporter, and Dr. Jay Bhattacharya, Professor of Medicine at Stanford University and co-author of the Great Barrington Declaration, discuss COVID lockdowns and the harm of closing schools, the latest on vaccines and vaccine distribution, the new COVID variants, masks (and double-masks), "focused protection," "trickle down epidemiology," overcoming COVID fear, the actual number of COVID deaths, COVID vs. the flu and more.
The Pandemic Has Erased Entire Categories of Friendship
https://www.theatlantic.com/health/archive/2021/01/pandemic-goodbye-casual-friends/617839/
A few months ago, when millions of Americans were watching the Netflix series Emily in Paris because it was what we had been given that week, I cued up the first episode and was beset almost immediately by an intense longing. Not for travel, or for opportunities to wear beautiful clothes—two commonly cited high points in an otherwise charmless show—but for sports. Specifically, watching sports in a packed bar, which is what the titular character’s boyfriend is doing when the viewer meets him.
The scene is fleeting, and it’s also pretty bad. It doesn’t come close to capturing the sweaty intensity of a horde of nervous fans, poised to embrace each other in collective joy or drink through despair. I know this because I am, sometimes unfortunately, a person who has spent a good chunk of her adult social life watching sports in bars, both with my actual close friends and with 500 or so fellow travelers at the New York City bar that hosts expatriated University of Georgia alumni during college-football season.
During the pandemic, I’ve been able to maintain, on an outdoor TV, the ability to watch a game with a couple of my closest buddies, which is a balm. But the other experience—the one Emily in Paris was trying to portray—has been lost entirely. In noticing all the ways the show misunderstood its joys, I realized how much I missed it, and especially how much I missed all of those people I only sort of know. Of the dozens of fellow fans and bar employees I’d greet with a hug on a normal fall Saturday, I follow only a handful of them on social media; for most of the others, I know only the first names, if that. But many comforted me through mutual, bone-deep disappointment, or sprayed champagne at me in exhilaration.
COVID-19 lockdowns are not worth the toll on our mental health
https://www.seattletimes.com/opinion/covid-19-lockdowns-are-not-worth-the-toll-on-our-mental-health/
Last February, the U.S. was ravaged by the coronavirus. A virus like no other, unknown to mankind. Our nation was met with an unimaginable disruption. It struck each individual like a ton of bricks. Lives were lost and some were spared. COVID-19 lockdowns were implemented in the hardest-hit cities. Many have willingly given up their freedom for the lockdowns. But are lockdowns worth it? Though we have spoken a lot about COVID-19 death rates, mandatory masking and social distancing, we rarely speak of those who suffer from depression and have fallen deeper into poverty.
Recently, the World Health Organization warned of the danger of lockdowns as they are “costly [and bring] social and economic life to a near stop.” Many experts, particularly in the United Kingdom, warn of the profound effects of lockdowns on both mental and physical health. Not only do they adversely affect health outcomes, but they also have a devastating impact on the nation’s economy. A survey conducted by the Centers for Disease Control shows a significant number of younger adults, essential workers and minorities have contemplated suicide during lockdowns. Depression rates tripled amid COVID-19 lockdowns, according to a study cited by the Center for Infectious Disease Research and Policy.
Research
Precision shielding for COVID-19: metrics of assessment and feasibility of deployment
https://www.nber.org/papers/w28264
Abstract:
The ability to preferentially protect high-risk groups in COVID-19 is hotly debated. Here, the aim is to present simple metrics of such precision shielding of people at high risk of death after infection by SARS-CoV-2; demonstrate how they can estimated; and examine whether precision shielding was successfully achieved in the first COVID-19 wave. The shielding ratio, S, is defined as the ratio of prevalence of infection among people in a high-risk group versus among people in a low-risk group. The contrasted risk groups examined here are according to age (≥70 vs <70 years), and institutionalised (nursing home) setting. For age-related precision shielding, data were used from large seroprevalence studies with separate prevalence data for elderly versus non-elderly and with at least 1000 assessed people≥70 years old. For setting-related precision shielding, data were analysed from 10 countries where information was available on numbers of nursing home residents, proportion of nursing home residents among COVID-19 deaths and overall population infection fatality rate (IFR). Across 17 seroprevalence studies, the shielding ratio S for elderly versus non-elderly varied between 0.4 (substantial shielding) and 1.6 (substantial inverse protection, that is, low-risk people being protected more than high-risk people). Five studies in the USA all yielded S=0.4–0.8, consistent with some shielding being achieved, while two studies in China yielded S=1.5–1.6, consistent with inverse protection. Assuming 25% IFR among nursing home residents, S values for nursing home residents ranged from 0.07 to 3.1. The best shielding was seen in South Korea (S=0.07) and modest shielding was achieved in Israel, Slovenia, Germany and Denmark. No shielding was achieved in Hungary and Sweden. In Belgium (S=1.9), the UK (S=2.2) and Spain (S=3.1), nursing home residents were far more frequently infected than the rest of the population. In conclusion, the experience from the first wave of COVID-19 suggests that different locations and settings varied markedly in the extent to which they protected high-risk groups. Both effective precision shielding and detrimental inverse protection can happen in real-life circumstances. COVID-19 interventions should seek to achieve maximal precision shielding.
Charts and Graphics
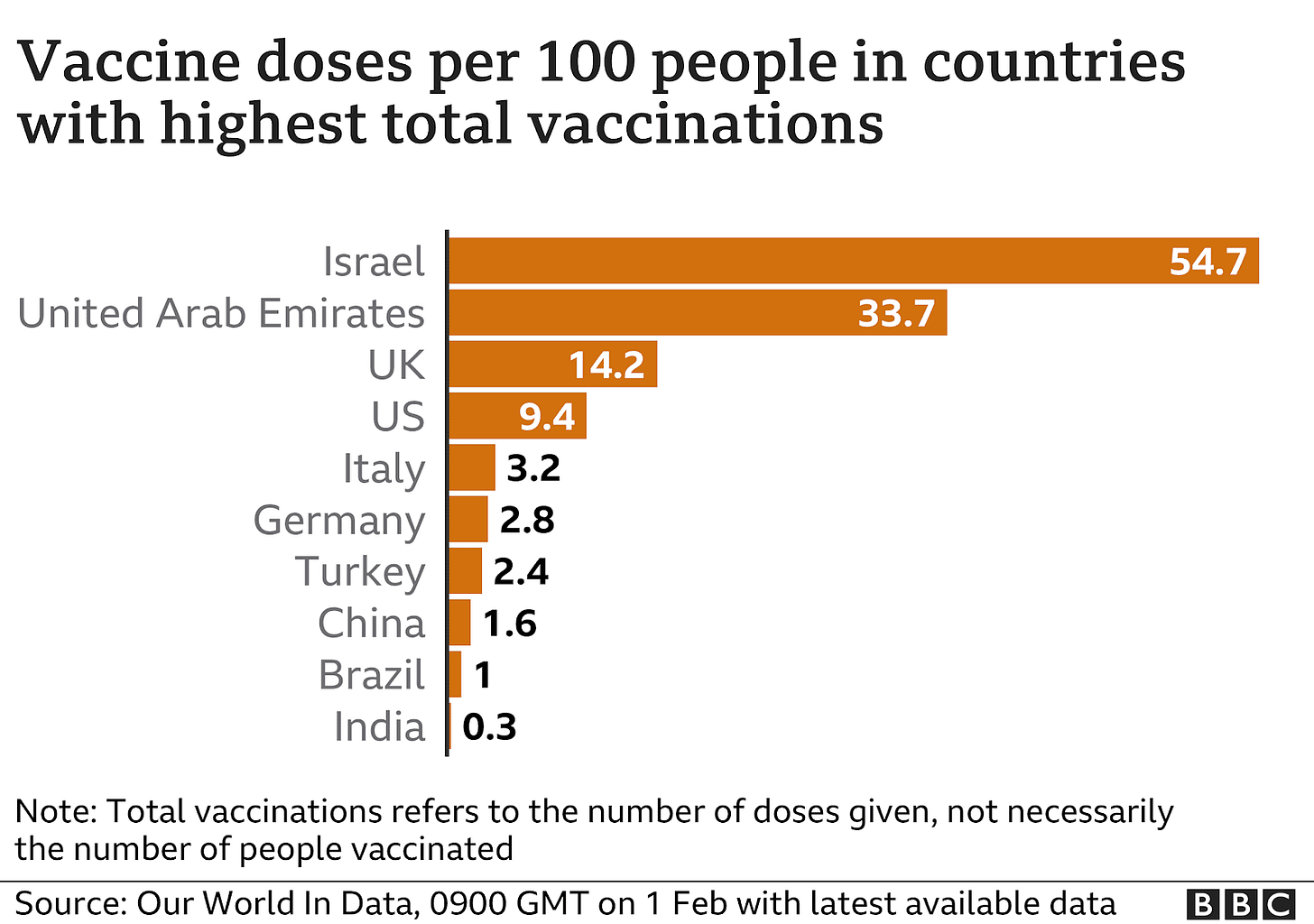
Economist Phil Magness: “It turns out that the UK and Sweden followed a similar pattern during both waves of the pandemic. They differed in levels of intensity, with the UK doing worse during both waves. This occurred despite the two countries taking completely opposite approaches to mitigation. At the end of the day, the lockdowners are going to have to explain how their favored policies yielded a worse outcome than seen in a country that rejected those policies despite having a parallel outbreak pattern.”
International News
Covid: Israel's vaccine rollout linked to infection fall
https://www.bbc.com/news/health-55706855
Israel's vaccination programme is showing signs of working to drive down infections and illness in the over-60s.
The fall appears to be most pronounced in older people and areas furthest ahead in their immunisation efforts.
This suggests it is the vaccine, and not just the country's current lockdown, taking effect.
Israeli Ministry of Health (MoH) figures show 531 over-60s, out of almost 750,000 fully vaccinated, tested positive for coronavirus (0.07%).
And far fewer fell ill, with 38 becoming hospitalised with moderate, severe or critical disease - a tiny proportion.
The MoH assessed the medical records of almost a million people in total - 743,845 of whom were over the age of 60 - until at least seven days after they received a second dose of the vaccine.
There were three deaths in vaccinated over-60s - although it is possible they contracted the infection earlier, before their immunity had time to build.