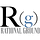Authoritarians Never Learn
In New York, unused vaccines go into the garbage as Governor Cuomo’s horrific mismanagement continues.
In other news:
A recent study shows people who have already contracted coronavirus are as protected against reinfection as those who have received the best COVID vaccine.
Drs. Vladimir Kogan and Vinay Prasad make an eloquent case for why public schools should stay open.
International authoritarianism remains in vogue:
Australia locked down Brisbane, its third-largest city, over a single new case of COVID.
China locked down two major cities over new COVID outbreaks. More than 22 million people in all have been ordered to remain inside their homes — double the number affected last January.
Interested in becoming knowledgeable on COVID? Become a premium member. Our premium members get special access to our personal data dashboards and analysis.
Want to support our work? Visit our Substack page and leave us a tip.
On Rational Ground for our premium members, our data analyses will always be available to you. Interested in becoming a COVID expert? Become a premium member.
Additionally, we just released an update on how COVID-19 is playing out on university campuses.
COVID News
Cuomo Fiddles with Vaccine while New York Burns
https://www.nationalreview.com/2021/01/cuomo-fiddles-with-vaccine-while-new-york-burns/
Andrew Cuomo forced vaccine doses to be thrown away. It can’t be stated often enough or loudly enough: After the miraculous and heroic efforts of great pharmaceutical companies to develop vaccines before the first American had even been infected, and after the usual testing and regulatory hurdles consumed nearly eleven months, and after the first New Yorker accepted her jab on December 14 in an event Cuomo celebrated and streamed on his official channel, the governor of New York has been preventing people from getting the vaccine. “Bedlam” and “chaos” are two of the more polite words being used by administrators on the ground as they tiptoe their way through the regulatory minefield Cuomo quickly engineered between health-care professionals and the people of New York.
Covid infection shown to provide as much immunity as vaccines
https://www.ft.com/content/929ef3cd-8611-49b2-9f23-918dc3470166
People who have already contracted coronavirus are as protected against reinfection as those who have received the best Covid-19 vaccines, according to a survey of 20,000 UK healthcare workers, the largest study in the world so far.
Public Health England regularly tested two matched groups of volunteers between June and November — 6,000 health workers who had previously been infected with coronavirus and 14,000 who had not.
A comparison of infections in the two groups, described in preliminary results released on Thursday, found that prior infection provided at least 83 per cent protection against reinfection. It gave better than 94 per cent protection against symptomatic Covid-19, matching the figures for the most effective Covid-19 vaccines.
Commentary/Analysis
After nine months, we still know masks don’t work
https://rationalground.com/after-nine-months-we-still-know-masks-dont-work/
Recently we highlighted an article by UF researchers that showed asymptomatic and presymptomatic spread of COVID-19 in households is essentially zero (0.7 ± 4.2 percent secondary attack rate). This result is important because potential asymptomatic spread was the basis for mask mandates across the country. Despite all the models and theories used to support non-pharmaceutical interventions (NPI), real-world evidence continues to show that these NPIs (mask mandates, lockdowns, etc.) are not effective.
Prior to COVID-19, the CDC’s Community Mitigation Guidelines to Prevent Pandemic Influenza (2017) said, “CDC does not routinely recommend the use of face masks by well persons in the home or other community settings as a means of avoiding infection” (p15). The document specifically talked about disposable surgical, medical, or dental procedure masks, not random cloth face masks. The document said that persons at high risk of complications (of flu) or who are caring for ill family members should wear masks but said, “little evidence supports the use of face masks by well persons in community settings” (p14).
In a January 28, 2020 press conference, Dr. Anthony Fauci said, “In all the history of respiratory-borne viruses of any type, asymptomatic transmission has never been the driver of outbreaks. The driver of outbreaks is always a symptomatic person. Even if there’s a rare asymptomatic person that might transmit, an epidemic is not driven by asymptomatic carriers.”
Even as late as April 6, the WHO’s guidelines said members of the general public “only need to wear a mask if you are taking care of a person with COVID-19” or “if you are coughing or sneezing.”
Op-Ed: Public Schools Should (Almost Always) Stay Open
https://www.medpagetoday.com/blogs/vinay-prasad/90658
Schools present a tradeoff. When they're open, society benefits from the essential services schools provide: education, child abuse reporting, hot meals, and socio-emotional development. Closing them may theoretically slow viral spread. How should a society decide?
Nearly every discussion or debate around COVID-19 has become protracted, political, and bitter, and what to do about schools is no exception. Over the last few months, we have reviewed the emerging evidence and reached the same conclusion: Unless the local healthcare system is approaching overload or collapse, schools should remain open. In this op-ed, we hope to explain why.
We approach this question from two very different perspectives -- one of us is a physician, epidemiologist, and public health scholar, and the other is a political scientist with a long-standing focus on education policy. Collectively, our expertise has allowed us to examine the tradeoffs of schools during a pandemic.
The Abuse of Science in the Corona Crisis
https://www.aier.org/article/the-abuse-of-science-in-the-corona-crisis/
Science plays a pivotal role in the current crisis, not only in investigating the nature of the virus, but also in guiding the political reactions to its spread.
Leopoldina, the German National Academy of Sciences, writes in a statement dated December 8, 2020:
Despite the prospect of a start of the vaccination campaign soon, it is absolutely necessary from a scientific point of view to quickly and drastically reduce the still clearly too high number of new infections through a hard lockdown.
With this document in her hands, the German chancellor, Angela Merkel, justified a hard lockdown in parliament on December 9, 2020, invoking laws of nature such as gravitation and the velocity of light as well as the force of enlightenment.
At least three things are remarkable about this document:
Research
Open Schools, Covid-19, and Child and Teacher Morbidity in Sweden
https://www.nejm.org/doi/full/10.1056/NEJMc2026670?query=TOC
In mid-March 2020, many countries decided to close schools in an attempt to limit the spread of severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2), the virus causing coronavirus disease 2019 (Covid-19). Sweden was one of the few countries that decided to keep preschools (generally caring for children 1 to 6 years of age) and schools (with children 7 to 16 years of age) open. Here, we present data from Sweden on Covid-19 among children 1 to 16 years of age and their teachers. In Sweden, Covid-19 was prevalent in the community during the spring of 2020.3 Social distancing was encouraged in Sweden, but wearing face masks was not.
Charts and Graphics
COVID-19 Vaccination Doses Administered Per Million People
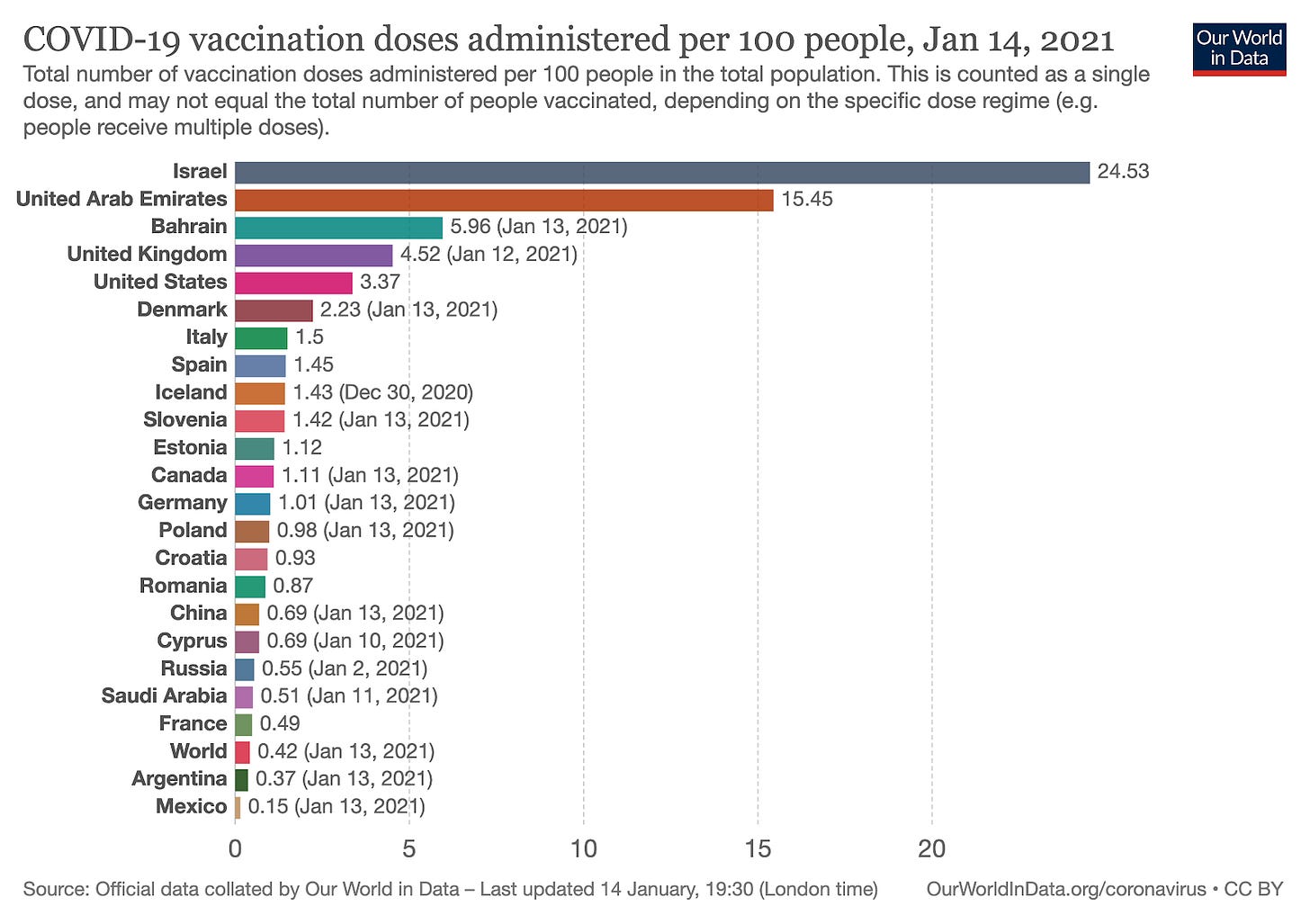
Florida - Daily New Cases Per 1 Million
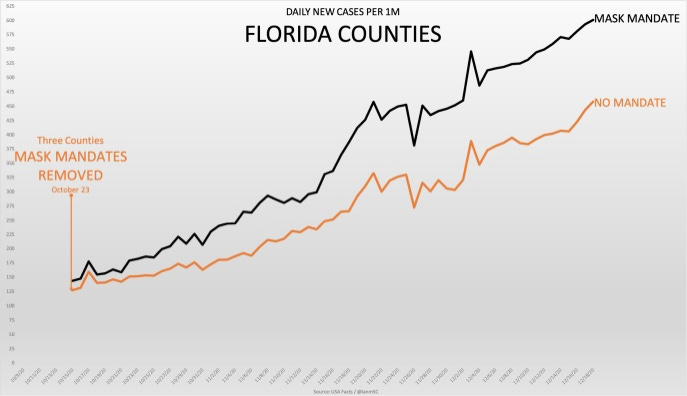
Kansas Contact Tracing
Kansas contact tracing data shows 0.91% of cases can be traced back to restaurants and bars, with 0 deaths resulting from them.
International News
Australia locks down city of 2 million over a single case of new COVID variant
Brisbane, Australia — Australia's third-largest city headed into lockdown and borders were set to tighten nationwide Friday, after a cleaner at a quarantine hotel contracted the U.K. coronavirus strain that officials say is more infectious. More than two million residents in the Greater Brisbane area will have to stay at home for at least three days from Friday evening, authorities said.
"If we are going to stop the spread of this infectious strain, this U.K. strain, we must act immediately," Queensland Premier Annastacia Palaszczuk told media.
Large lines formed at shops around the city, prompting officials to urge people to stop panic-buying. The incoming restrictions will still allow residents to leave home to buy essentials.
Facing New Outbreaks, China Places Over 22 Million on Lockdown
https://www.nytimes.com/2021/01/13/world/asia/china-covid-lockdown.html
When a handful of new coronavirus cases materialized this month in a province surrounding Beijing — apparently spread at a village wedding party — the Chinese authorities bolted into action.
They locked down two cities with more than 17 million people, Shijiazhuang and Xingtai. They ordered a crash testing regime of nearly every resident there, which was completed in a matter of days.
They shut down transportation and canceled weddings, funerals and, most significantly, a provincial Communist Party conference.
By this week the lockdowns expanded to include another city on the edge of Beijing, Langfang, as well as a county in Heilongjiang, a northeastern province. Districts in Beijing itself, the Chinese capital, also shut down.